1.3.9. More About Vitamins
Introduction
Vitamins are obtained from the different types of foods that we consume. If a diet is lacking a certain type of nutrient, a vitamin deficiency may occur. Vitamins are organic compounds that are traditionally assigned to two groups fat-soluble (hydrophobic) or water-soluble (hydrophilic). This classification determines where they act in the body. Water-soluble vitamins act in the cytosol of cells or in extracellular fluids such as blood; fat-soluble vitamins are largely responsible for protecting cell membranes from free radical damage. The body can synthesize some vitamins, but others must be obtained from the diet.
Figure 1.3.9.1 The Vitamins
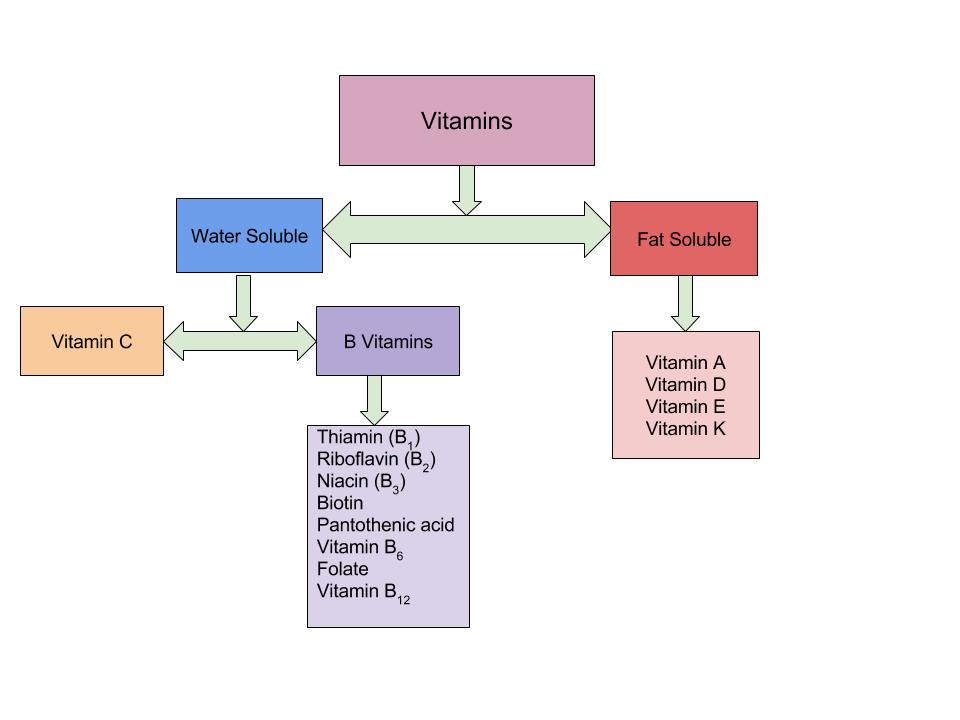
One major difference between fat-soluble vitamins and water-soluble vitamins is the way they are absorbed in the body. Vitamins are absorbed primarily in the small intestine and their bioavailability is dependent on the food composition of the diet. Fat-soluble vitamins are absorbed along with dietary fat. Therefore, if a meal is very low in fat, the absorption of the fat-soluble vitamins will be impaired. Once fat-soluble vitamins have been absorbed in the small intestine, they are packaged and incorporated along with other fatty acids and transported in the lymphatic system to the liver. Water-soluble vitamins on the other hand are absorbed in the small intestine but are transported to the liver through blood vessels. (Figure 1.3.9.2 “Absorption of Fat-Soluble and Water-Soluble Vitamins”).
Figure 1.3.9.2 Absorption of Fat-Soluble and Water-Soluble Vitamins
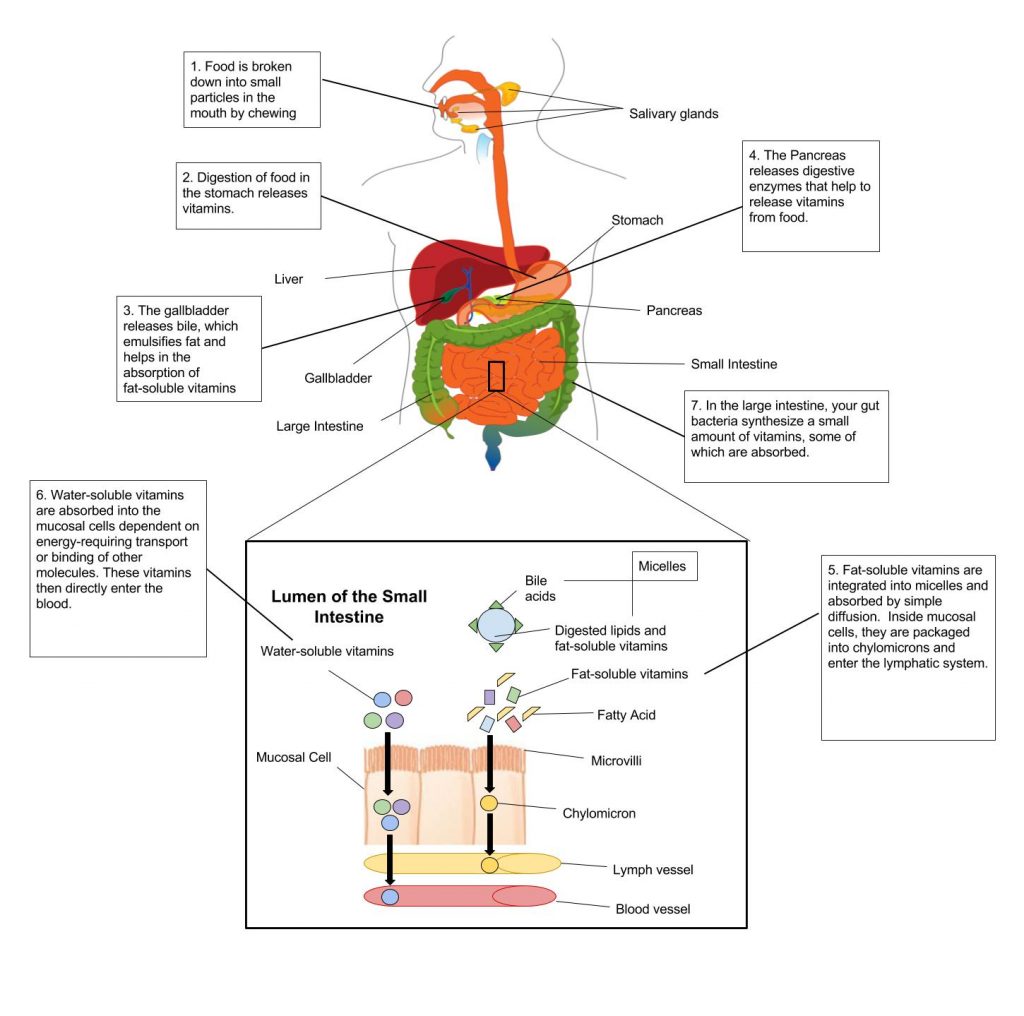
Fat-Soluble Vitamins
Vitamin A
Vitamin A is a generic term for a group of similar compounds called retinoids. Retinol is the form of vitamin A found in animal-derived foods, and is converted in the body to the biologically active forms of vitamin A: retinal and retinoic acid (thus retinol is sometimes referred to as “preformed vitamin A”). About 10 percent of plant-derived carotenoids, including beta-carotene, can be converted in the body to retinoids and are another source of functional vitamin A. Carotenoids are pigments synthesized by plants that give them their yellow, orange, and red color. Over six hundred carotenoids have been identified and, with just a few exceptions, all are found in the plant kingdom. There are two classes of carotenoids—the xanthophylls, which contain oxygen, and the carotenes, which do not.
In plants, carotenoids absorb light for use in photosynthesis and act as antioxidants. Many biological actions of carotenoids are attributed to their antioxidant activity, but they likely act by other mechanisms, too.
Vitamin A is fat-soluble and is packaged into chylomicrons in small intestine, and transported to the liver. The liver stores and exports vitamin A as needed; it is released into the blood bound to a retinol-binding protein, which transports it to cells. Carotenoids are not absorbed as well as vitamin A, but similar to vitamin A, they do require fat in the meal for absorption. In intestinal cells, carotenoids are packaged into the lipid-containing chylomicrons inside small intestine mucosal cells and then transported to the liver. In the liver, carotenoids are repackaged into lipoproteins, which transport them to cells.
The retinoids are aptly named as their most notable function is in the retina of the eye where they aid in vision, particularly in seeing under low-light conditions. This is why night blindness is the most definitive sign of vitamin A deficiency. Vitamin A has several important functions in the body, including maintaining vision and a healthy immune system. Many of vitamin A’s functions in the body are similar to the functions of hormones (for example, vitamin A can interact with DNA, causing a change in protein function). Vitamin A assists in maintaining healthy skin and the linings and coverings of tissues; it also regulates growth and development. As an antioxidant, vitamin A protects cellular membranes, helps in maintaining glutathione levels, and influences the amount and activity of enzymes that detoxify free radicals.
Vision
Retinol that is circulating in the blood is taken up by cells in the eye retina, where it is converted to retinal and is used to help the pigment rhodopsin, which is involved in the eye’s ability to see under low light conditions. A deficiency in vitamin A thus results in less rhodopsin and a decrease in the detection of low-level light, a condition referred to as night-blindness.
Insufficient intake of dietary vitamin A over time can also cause complete vision loss. In fact, vitamin A deficiency is the number one cause of preventable blindness worldwide. Vitamin A not only supports the vision function of eyes but also maintains the coverings and linings of the eyes. Vitamin A deficiency can lead to the dysfunction of the linings and coverings of the eye (eg. Bitot spots), causing dryness of the eyes, a condition called xerophthalmia. The progression of this condition can cause ulceration of the cornea and eventually blindness.
Figure 1.3.9.3 Bitot Spot Caused by Vitamin A Deficiency

Figure 1.3.9.4 Vitamin A Deficiency World Map
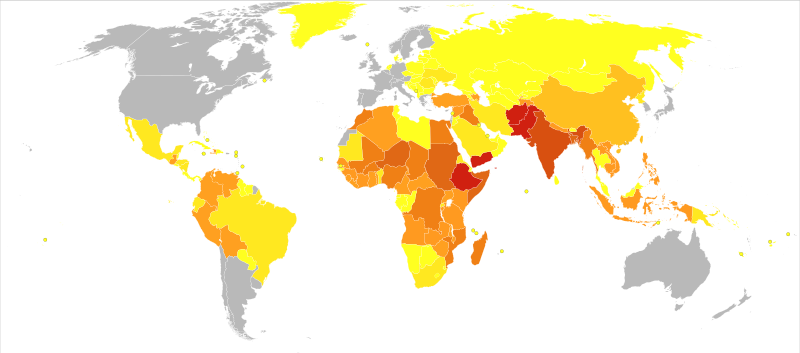

Immunity
In the twenty-first century, science has demonstrated that vitamin A greatly affects the immune system. What we are still lacking are clinical trials investigating the proper doses of vitamin A required to help ward off infectious disease and how large of an effect vitamin A supplementation has on populations that are not deficient in this vitamin. This brings up one of our common themes in this text—micronutrient deficiencies may contribute to the development, progression, and severity of a disease, but this does not mean that an increased intake of these micronutrients will solely prevent or cure disease. The effect, as usual, is cumulative and depends on the diet as a whole, among other things.
Growth and Development
Vitamin A acts similarly to some hormones in that it is able to change the amount of proteins in cells by interacting with DNA. This is the primary way that vitamin A affects growth and development. Vitamin A deficiency in children is linked to growth retardation; however, vitamin A deficiency is often accompanied by protein malnutrition and iron deficiency, thereby confounding the investigation of vitamin A’s specific effects on growth and development.
In the fetal stages of life, vitamin A is important for limb, heart, eye, and ear development and in both deficiency and excess, vitamin A causes birth defects. Furthermore, both males and females require vitamin A in the diet to effectively reproduce.
Vitamin A Toxicity
Vitamin A toxicity, or hypervitaminosis A, is rare. Typically it requires you to ingest ten times the RDA of preformed vitamin A in the form of supplements (it would be hard to consume such high levels from a regular diet) for a substantial amount of time, although some people may be more susceptible to vitamin A toxicity at lower doses. The signs and symptoms of vitamin A toxicity include dry, itchy skin, loss of appetite, swelling of the brain, and joint pain. In severe cases, vitamin A toxicity may cause liver damage and coma.
Vitamin A is essential during pregnancy, but doses above 3,000 micrograms per day (10,000 international units) have been linked to an increased incidence of birth defects. Pregnant women should check the amount of vitamin A contained in any prenatal or pregnancy multivitamin she is taking to assure the amount is below the UL.
Dietary Sources of Vitamin A and Beta-Carotene
Preformed vitamin A is found only in foods from animals, with the liver being the richest source because that’s where vitamin A is stored (see Table 1.3.9.1 “Vitamin A Content of Various Foods”). The dietary sources of carotenoids will be given in the following text.
Table 1.3.9.1 Vitamin A Content of Various Foods
| Food | Serving | Vitamin A (IU) | Percent Daily Value |
| Beef liver | 3 oz. | 27,185 | 545 |
| Chicken liver | 3 oz. | 12,325 | 245 |
| Milk, skim | 1 c. | 500 | 10 |
| Milk, whole | 1 c. | 249 | 5 |
| Cheddar cheese | 1 oz. | 284 | 6 |
Source: Dietary Supplement Fact Sheet: Vitamin A. Office of Dietary Supplements, National Institutes of Health. http://ods.od.nih.gov/factsheets/VitaminA-QuickFacts/. Updated September 5, 2012. Accessed October 7, 2017.
Table 1.3.9.2 Alpha- and Beta-Carotene Content of Various Foods
| Food | Serving | Beta-carotene (mg) | Alpha-carotene (mg) |
| Pumpkin, canned | 1c. | 17.00 | 11.70 |
| Carrot juice | 1c. | 22.00 | 10.20 |
| Carrots, cooked | 1c. | 13.00 | 5.90 |
| Carrots, raw | 1 medium | 5.10 | 2.10 |
| Winter squash, baked | 1c. | 5.70 | 1.40 |
| Collards, cooked | 1c. | 11.60 | 0.20 |
| Tomato | 1 medium | 0.55 | 0.10 |
| Tangerine | 1 medium | 0.13 | 0.09 |
| Peas, cooked | 1c. | 1.20 | 0.09 |
Source: USDA National Nutrient Database for Standard Reference, Release 23. Agricultural Research Service, U.S., Department of Agriculture,. http://www.ars.usda.gov/ba/bhnrc/ndl. Updated: October 22, 2017. Accessed: August 31, 2021.
Vitamin D
Vitamin D refers to a group of fat-soluble vitamins derived from cholesterol. Vitamins D2 (ergocalciferol) and D3 (calcitriol) are the only ones known to have biological actions in the human body. The skin synthesizes vitamin D when exposed to sunlight. In fact, for most people, more than 90 percent of their vitamin D3 comes from the casual exposure to the UVB rays in sunlight. Anything that reduces your exposure to the sun’s UVB rays decreases the amount of vitamin D3 your skin synthesizes. That would include long winters, your home’s altitude, whether you are wearing sunscreen, and the color of your skin (including tanned skin). Do you ever wonder about an increased risk for skin cancer by spending too much time in the sun? Do not fret. Less than thirty minutes of sun exposure to the arms and legs will increase blood levels of vitamin D3 more than orally taking 10,000 IU (250 micrograms) of vitamin D3.
Figure 1.3.9.5 The Functions of Vitamin D
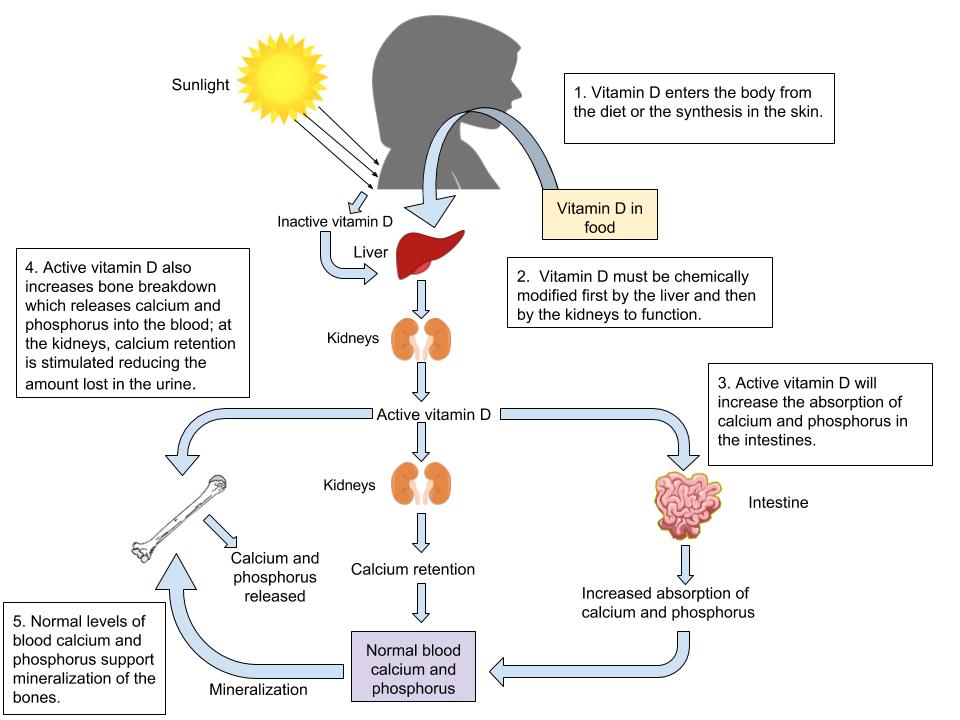
Vitamin D’s Functional Role
Activated vitamin D3 (calcitriol) regulates blood calcium levels in concert with parathyroid hormone. In the absence of an adequate intake of vitamin D, less than 15 percent of calcium is absorbed from foods or supplements. The effects of calcitriol on calcium homeostasis are critical for bone health. A deficiency of vitamin D in children causes the bone disease nutritional rickets. Rickets is very common among children in developing countries and is characterized by soft, weak, deformed bones that are exceptionally susceptible to fracture. In adults, vitamin D deficiency causes a similar disease called osteomalacia, which is characterized by low BMD. Osteomalacia has the same symptoms and consequences as osteoporosis and often coexists with osteoporosis. Vitamin D deficiency is common, especially in the elderly population, dark-skinned populations, and in the many people who live in the northern latitudes where sunlight exposure is much decreased during the long winter season.
Figure 1.3.9.6 Rickets in Children

Health Benefits
Observational studies have shown that people with low levels of vitamin D in their blood have lower BMD and an increased incidence of osteoporosis. In contrast, diets with high intakes of salmon, which contains a large amount of vitamin D, are linked with better bone health. A review of twelve clinical trials, published in the May 2005 issue of the Journal of the American Medical Association, concluded that oral vitamin D supplements at doses of 700–800 international units per day, with or without coadministration of calcium supplements, reduced the incidence of hip fracture by 26 percent and other nonvertebral fractures by 23 percent.[1] A reduction in fracture risk was not observed when people took vitamin D supplements at doses of 400 international units.
Many other health benefits have been linked to higher intakes of vitamin D, from decreased cardiovascular disease to the prevention of infection. Furthermore, evidence from laboratory studies conducted in cells, tissues, and animals suggest vitamin D prevents the growth of certain cancers, blocks inflammatory pathways, reverses atherosclerosis, increases insulin secretion, and blocks viral and bacterial infection and many other things. Vitamin D deficiency has been linked to an increased risk for autoimmune diseases. Immune diseases, rheumatoid arthritis, multiple sclerosis, and Type 1 diabetes have been observed in populations with inadequate vitamin D levels. Additionally, vitamin D deficiency is linked to an increased incidence of hypertension. Until the results come out from the VITAL study, the bulk of scientific evidence touting other health benefits of vitamin D is from laboratory and observational studies and requires confirmation in clinical intervention studies.
Vitamin D Toxicity
Although vitamin D toxicity is rare, too much can cause high levels of calcium concentrations or hypercalcemia. Hypercalcemia can lead to a large amount of calcium to be excreted through the urine which can cause kidney damage. Calcium deposits may also develop in soft tissues such as the kidneys, blood vessels, or other parts of the cardiovascular system. However, it is important to know that the synthesis of vitamin D from the sun does not cause vitamin D toxicity due to the skin production of vitamin D3 being a tightly regulated process.
Toxicity from excess vitamin D is rare, but certain diseases such as hyperparathyroidism, lymphoma, and tuberculosis make people more sensitive to the increases in calcium caused by high intakes of vitamin D.
Dietary Sources of Vitamin D
Table 1.3.9.3 Vitamin D Content of Various Foods
| Food | Serving | Vitamin D (IU) | Percent daily value |
| Swordfish | 3 oz. | 566 | 142 |
| Salmon | 3 oz. | 447 | 112 |
| Tuna fish, canned in water, drained | 3 oz. | 154 | 39 |
| Orange juice fortified with vitamin D | 1 c. | 137 | 34 |
| Milk, nonfat, reduced fat, and whole, vitamin D- fortified | 1 c. | 115-124 | 29-31 |
| Margarine, fortified | 1 tbsp. | 60 | 15 |
| Sardines, canned in oil, drained | 2 e. | 46 | 12 |
| Beef liver | 3 oz. | 42 | 11 |
| Egg, large | 1 e. | 41 | 10 |
Source: Dietary Supplement Fact Sheet: Vitamin D. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/#h3. Updated September 5, 2012. Accessed October 22, 2017.
Vitamin E
Vitamin E occurs in eight chemical forms, of which alpha-tocopherol appears to be the only form that is recognized to meet human requirements. Alpha-tocopherol and vitamin E’s other constituents are fat-soluble and primarily responsible for protecting cell membranes against lipid destruction caused by free radicals, therefore making it an antioxidant. When alpha-tocopherol interacts with a free radical it is no longer capable of acting as an antioxidant unless it is enzymatically regenerated. Vitamin C helps to regenerate some of the alpha-tocopherol, but the remainder is eliminated from the body. Therefore, to maintain vitamin E levels, you ingest it as part of your diet.
Insufficient levels are rare (signs and symptoms of such conditions are not always evident) but are primarily the result of nerve degeneration. People with malabsorption disorders, such as Crohn’s disease or cystic fibrosis, and babies born prematurely, are at higher risk for vitamin E deficiency.
Vitamin E has many other important roles and functions in the body such as boosting the immune system by helping to fight off bacteria and viruses. It also enhances the dilation of blood vessels and inhibiting the formation of blood clotting. Despite vitamin E’s numerous beneficial functions when taken in recommended amounts, large studies do not support the idea that taking higher doses of this vitamin will increase its power to prevent or reduce disease risk.[2][3]
Fat in the diet is required for vitamin E absorption as it is packaged into lipid-rich chylomicrons in intestinal cells and transported to the liver. The liver stores some of the vitamin E or packages it into lipoproteins, which deliver it to cells.
Eye Conditions
Oxidative stress plays a role in age-related loss of vision, called macular degeneration. Age-related macular degeneration (AMD) primarily occurs in people over age fifty and is the progressive loss of central vision resulting from damage to the center of the retina, referred to as the macula. There are two forms of AMD, dry and wet, with wet being the more severe form.
In the dry form, deposits form in the macula; the deposits may or may not directly impair vision, at least in the early stages of the disease. In the wet form, abnormal blood vessel growth in the macula causes vision loss. Clinical trials evaluating the effects of vitamin E supplements on AMD and cataracts (clouding of the lens of an eye) did not consistently observe a decreased risk for either. However, scientists do believe vitamin E in combination with other antioxidants such as zinc and copper may slow the progression of macular degeneration in people with early-stage disease.
Dementia
The brain’s high glucose consumption makes it more vulnerable than other organs to oxidative stress. Oxidative stress has been implicated as a major contributing factor to dementia and Alzheimer’s disease. Some studies suggest vitamin E supplements delay the progression of Alzheimer’s disease and cognitive decline, but again, not all of the studies confirm the relationship. A recent study with over five thousand participants published in the July 2010 issue of the Archives of Neurology demonstrated that people with the highest intakes of dietary vitamin E were 25 percent less likely to develop dementia than those with the lowest intakes of vitamin E.[4]
More studies are needed to better assess the dose and dietary requirements of vitamin E and, for that matter, whether other antioxidants lower the risk of dementia, a disease that not only devastates the mind, but also puts a substantial burden on loved ones, caretakers, and society in general.
Vitamin E Toxicity
Currently, researchers have not found any adverse effects from consuming vitamin E in food. Although that may be the case, supplementation of alpha-tocopherol in animals has shown to cause hemorrhage and disrupt blood coagulation. Extremely high levels of vitamin E can interact with vitamin K-dependent clotting factors causing an inhibition of blood clotting.[5]
Vitamin E supplements often contain more than 400 international units, which is almost twenty times the RDA. The UL for vitamin E is set at 1,500 international units for adults. There is some evidence that taking vitamin E supplements at high doses has negative effects on health. As mentioned, vitamin E inhibits blood clotting and a few clinical trials have found that people taking vitamin E supplements have an increased risk of stroke. In contrast to vitamin E from supplements, there is no evidence that consuming foods containing vitamin E compromises health.
Dietary Sources of Vitamin E
Add some nuts to your salad and make your own dressing to get a healthy dietary dose of vitamin E.

Vitamin E is found in many foods, especially those higher in fat, such as nuts and oils. Some spices, such as paprika and red chili pepper, and herbs, such as oregano, basil, cumin, and thyme, also contain vitamin E. (Keep in mind spices and herbs are commonly used in small amounts in cooking and therefore are a lesser source of dietary vitamin E.) See Table 1.3.9.4 “Vitamin E Content of Various Foods” for a list of foods and their vitamin E contents.
Everyday Connection
To increase your dietary intake of vitamin E from plant-based foods try a spinach salad with tomatoes and sunflower seeds, and add a dressing made with sunflower oil, oregano, and basil. The oil from the sunflower seeds and oil will aid in the absorption of vitamin E from the spinach and tomatoes.
Table 1.3.9.4 Vitamin E Content of Various Foods
| Food | Serving size | Vitamin E (mg) | Percent daily value |
| Sunflower seeds | 1 oz. | 7.4 | 37 |
| Almonds | 1 oz. | 6.8 | 34 |
| Sunflower oil | 1 Tbsp | 5.6 | 28 |
| Hazelnuts 1 oz. | 1 oz. | 4.3 | 22 |
| Peanut butter | 2 Tbsp. | 2.9 | 15 |
| Peanuts 1 oz. | 1 oz. | 2.2 | 11 |
| Corn oil 1 Tbsp. | 1 Tbsp. | 1.9 | 10 |
| Kiwi | 1 medium | 1.1 | 6 |
| Tomato | 1 medium | 0.7 | 4 |
| Spinach | 1 c. raw | 0.6 | 3 |
Source: Dietary Supplement Fact Sheet: Vitamin E.Office of Dietary Supplements, National Institutes of Health. http://ods.od.nih.gov/factsheets/VitaminE-QuickFacts/. Updated October 11, 2011. Accessed October 5, 2017.
Vitamin K
Vitamin K refers to a group of fat-soluble vitamins that are similar in chemical structure. Vitamin K is critical for blood function acting as coenzymes which play an essential role in blood coagulation (aka blood clotting). Blood-clotting proteins are continuously circulating in the blood. Upon injury to a blood vessel, platelets stick to the wound forming a plug. Without vitamin K, blood would not clot.
A deficiency in vitamin K causes bleeding disorders. It is relatively rare, but people who have liver or pancreatic disease, celiac disease, or malabsorption conditions are at higher risk for vitamin K deficiency. Signs and symptoms include nosebleeds, easy bruising, broken blood vessels, bleeding gums, and heavy menstrual bleeding in women. The function of the anticoagulant drug warfarin is impaired by excess vitamin K intake from supplements. Calcium additionally plays a role in activation of blood-clotting proteins.
Bone Health
Vitamin K is also required for maintaining bone health. It modifies the protein osteocalcin, which is involved in the bone remodeling process. All the functions of osteocalcin and the other vitamin K-dependent proteins in bone tissue are not well understood and are under intense study. Some studies do show that people who have diets low in vitamin K also have an increased risk for bone fractures.
Dietary Sources of Vitamin K
Vitamin K is present in many foods. It is found in highest concentrations in green vegetables such as broccoli, cabbage, kale, parsley, spinach, and lettuce. Additionally, vitamin K can be synthesized via bacteria in the large intestine. The exact amount of vitamin K synthesized by bacteria that is actually absorbed in the lower intestine is not known, but likely contributes less than 10 percent of the recommended intake. Newborns have low vitamin K stores and it takes time for the sterile newborn gut to acquire the good bacteria it needs to produce vitamin K. So, it has become a routine practice to inject newborns with a single intramuscular dose of vitamin K. This practice has basically eliminated vitamin K-dependent bleeding disorders in babies.
Table 1.3.9.5 Dietary Sources of Vitamin K
| Food | Serving | Vitamin K (mcg) | Percent daily value |
| Broccoli | ½ c. | 160 | 133 |
| Asparagus | 4 spears | 34 | 28 |
| Cabbage | ½ c. | 56 | 47 |
| Spinach | ½ c. | 27 | 23 |
| Green peas | ½ c. | 16 | 13 |
| Cheese | 1 oz. | 10 | 8 |
| Ham | 3 oz. | 13 | 11 |
| Ground beef | 3 oz. | 6 | 5 |
| Bread | 1 slice | 1.1 | <1 |
| Orange | 1 e. | 1.3 | 1 |
Source: National Institutes of Health. https://ods.od.nih.gov/factsheets/VitaminK-Consumer/#h3. Updated on Feb 24, 2020. Accessed on Nov 14, 2020.
Water-Soluble Vitamins
All water-soluble vitamins play a different kind of role in energy metabolism; they are required as functional parts of enzymes involved in energy release and storage. Vitamins and minerals that make up part of enzymes are referred to as coenzymes and cofactors, respectively. Coenzymes and cofactors are required by enzymes to catalyze a specific reaction. They assist in converting a substrate to an end-product. Coenzymes and cofactors are essential in catabolic pathways and play a role in many anabolic pathways too.
In addition to being essential for metabolism, many vitamins and minerals are required for blood renewal and function. At insufficient levels in the diet these vitamins and minerals impair the health of blood and consequently the delivery of nutrients in and wastes out, among many other functions. In this section we will focus on the vitamins that take part in metabolism and blood function and renewal.
Figure 1.3.9.7 Enzyme Active Site for Cofactors
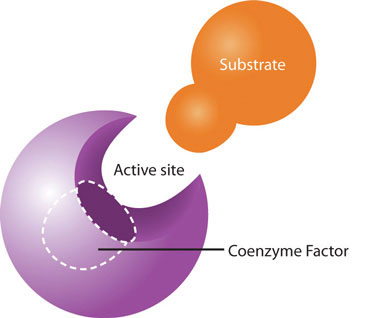
Source: Water-Soluble Vitamins.
Vitamin C
Vitamin C, also commonly called ascorbic acid, is a water-soluble micronutrient essential in the diet for humans, although most other mammals can readily synthesize it. Vitamin C’s ability to easily donate electrons makes it a highly effective antioxidant. It is effective in scavenging reactive oxygen species, reactive nitrogen species, and many other free radicals. It protects lipids both by disabling free radicals and by aiding in the regeneration of vitamin E.
In addition to its role as an antioxidant, vitamin C is a required part of several enzymes like signaling molecules in the brain, some hormones, and amino acids. Vitamin C is also essential for the synthesis and maintenance of collagen. Collagen is the most abundant protein in the body and used for different functions such as the structure for ligaments, tendons, and blood vessels and also scars that bind wounds together. Vitamin C acts as the glue that holds the collagen fibers together and without sufficient levels in the body, collagen strands are weak and abnormal (see Figure 1.3.9.8. “The Role of Vitamin C in Collagen Synthesis”).
Figure 1.3.9.8 The Role of Vitamin C in Collagen Synthesis
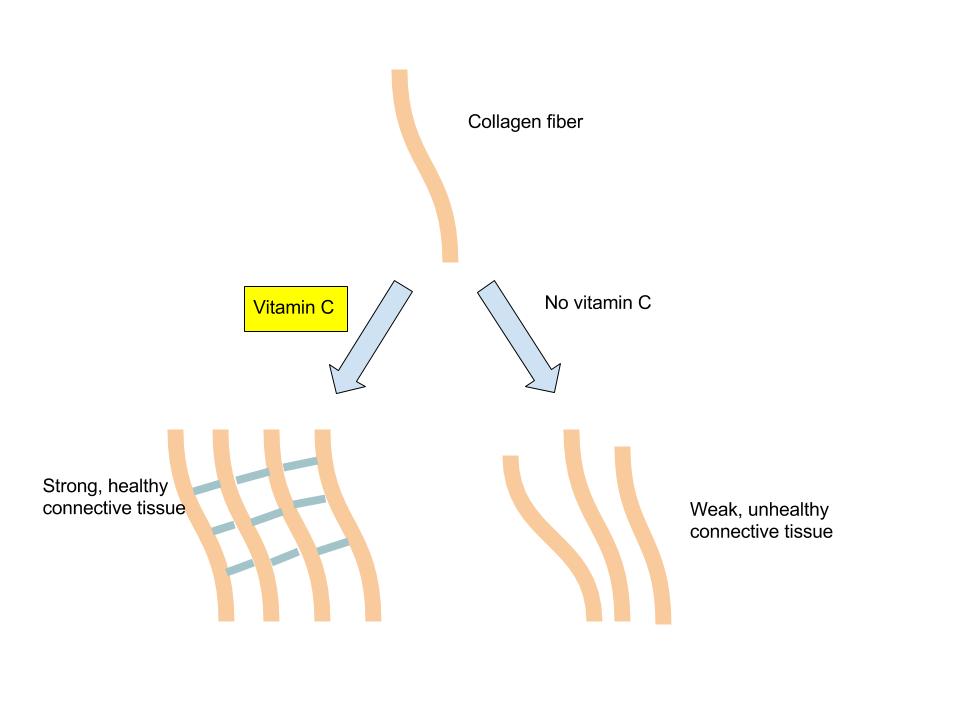
Vitamin C levels in the body are affected by the amount in the diet, which influences how much is absorbed and how much the kidney allows to be excreted, such that the higher the intake, the more vitamin C is excreted. Vitamin C is not stored in any significant amount in the body, but once it has reduced a free radical, it is very effectively regenerated and therefore it can exist in the body as a functioning antioxidant for many weeks.
The classic condition associated with vitamin C deficiency is scurvy. The signs and symptoms of scurvy include skin disorders, bleeding gums, painful joints, weakness, depression, and increased susceptibility to infections. Scurvy is prevented by having an adequate intake of fruits and vegetables rich in vitamin C.
Figure 1.3.9.9 Bleeding Gums Associated with Scurvy
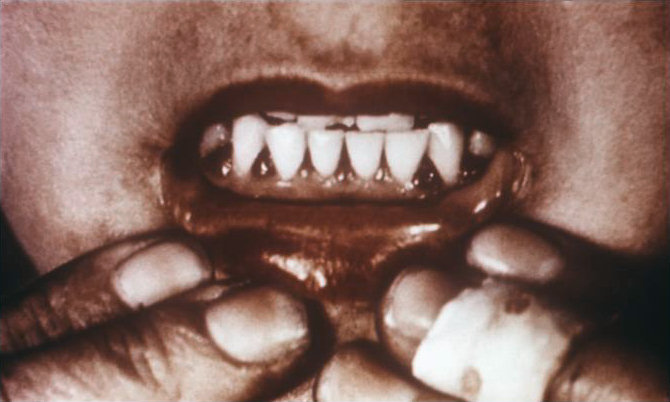
Source: Water-Soluble Vitamins.
Cardiovascular Disease
Vitamin C’s ability to prevent disease has been debated for many years. Overall, higher dietary intakes of vitamin C (via food intake, not supplements), are linked to decreased disease risk. A review of multiple studies published in the April 2009 issue of the Archives of Internal Medicine concludes there is moderate scientific evidence supporting the idea that higher dietary vitamin C intakes are correlated with reduced cardiovascular disease risk, but there is insufficient evidence to conclude that taking vitamin C supplements influences cardiovascular disease risk.[6] Vitamin C levels in the body have been shown to correlate well with fruit and vegetable intake, and higher plasma vitamin C levels are linked to reduced risk of some chronic diseases. In a study involving over twenty thousand participants, people with the highest levels of circulating vitamin C had a 42 percent decreased risk for having a stroke.[7]
Cancer
There is some evidence that a higher vitamin C intake is linked to a reduced risk of cancers of the mouth, throat, esophagus, stomach, colon, and lung, but not all studies confirm this is true. As with the studies on cardiovascular disease, the reduced risk of cancer is the result of eating foods rich in vitamin C, such as fruits and vegetables, not from taking vitamin C supplements. In these studies, the specific protective effects of vitamin C cannot be separated from the many other beneficial chemicals in fruits and vegetables.
Immunity
Vitamin C does have several roles in the immune system, and many people increase vitamin C intake either from diet or supplements when they have a cold. Many others take vitamin C supplements routinely to prevent colds. Contrary to this popular practice, however, there is no good evidence that vitamin C prevents a cold. A review of more than fifty years of studies published in 2004 in the Cochrane Database of Systematic Reviews concluded that taking vitamin C routinely does not prevent colds in most people, but it does slightly reduce cold severity and duration. Moreover, taking megadoses (up to 4 grams per day) at the onset of a cold provides no benefits.[8]
Gout is a disease caused by elevated circulating levels of uric acid and is characterized by recurrent attacks of tender, hot, and painful joints. There is some evidence that a higher intake of vitamin C reduces the risk of gout.
Vitamin C Toxicity
High doses of vitamin C have been reported to cause numerous problems, but the only consistently shown side effects are gastrointestinal upset and diarrhea. To prevent these discomforts the IOM has set a UL for adults at 2,000 milligrams per day (greater than twenty times the RDA).
At very high doses in combination with iron, vitamin C has sometimes been found to increase oxidative stress, reaffirming that getting your antioxidants from foods is better than getting them from supplements, as that helps regulate your intake levels. There is some evidence that taking vitamin C supplements at high doses increases the likelihood of developing kidney stones, however, this effect is most often observed in people that already have multiple risk factors for kidney stones.
Dietary Sources of Vitamin C
Citrus fruits are great sources of vitamin C and so are many vegetables. In fact, British sailors in the past were often referred to as “limeys” as they carried sacks of limes onto ships to prevent scurvy. Vitamin C is not found in significant amounts in animal-based foods.
Because vitamin C is water-soluble, it leaches away from foods considerably during cooking, freezing, thawing, and canning. Up to 50 percent of vitamin C can be boiled away. Therefore, to maximize vitamin C intake from foods, you should eat fruits and vegetables raw or lightly steamed. For the vitamin C content of various foods, see Table 1.3.9.6 “Vitamin C Content of Various Foods.”
Table 1.3.9.6 Vitamin C Content of Various Foods
| Food | Serving | Vitamin C (mg) | Percent daily value |
| Orange juice | 6 oz. | 93 | 155 |
| Grapefruit juice | 6 oz. | 70 | 117 |
| Orange | 1 medium | 70 | 117 |
| Strawberries | 1 c. | 85 | 164 |
| Tomato | 1 medium | 17 | 28 |
| Sweet red pepper | ½ c. raw | 95 | 158 |
| Broccoli | ½ c. cooked | 51 | 65 |
| Romaine lettuce | 2 c. | 28 | 47 |
| Cauliflower | 1 c. boiled | 55 | 86 |
| Potato | 1 medium, baked | 17 | 28 |
Source: Dietary Supplement Fact Sheet: Vitamin C. Office of Dietary Supplements, National Institutes of Health. http://ods.od.nih.gov/factsheets/VitaminC-QuickFacts/. Updated June 24, 2011. Accessed October 5, 2017.
Thiamin (B1 )
Thiamin is especially important in glucose metabolism. It acts as a cofactor for enzymes that break down glucose for energy production. Thiamin plays a key role in nerve cells as the glucose that is catabolized by thiamin is needed for an energy source. Additionally, thiamin plays a role in the synthesis of neurotransmitters and is therefore required for RNA, DNA, and ATP synthesis.
The brain and heart are most affected by a deficiency in thiamin. Thiamin deficiency, also known as beriberi, can cause symptoms of fatigue, confusion, movement impairment, pain in the lower extremities, swelling, and heart failure. It is prevalent in societies whose main dietary staple is white rice. During the processing of white rice, the bran is removed, along with what were called in the early nineteenth century, “accessory factors,” that are vital for metabolism.
Another common thiamin deficiency known as Wernicke- Korsakoff syndrome can cause similar symptoms as beriberi such as confusion, loss of coordination, vision changes, hallucinations, and may progress to coma and death. This condition is specific to alcoholics as diets high in alcohol can cause thiamin deficiency. Other individuals at risk include individuals who also consume diets typically low in micronutrients such as those with eating disorders, elderly, and individuals who have gone through gastric bypass surgery.[9]
Dietary Sources
Whole grains, meat and fish are great sources of thiamin. The United States as well as many other countries, fortify their refined breads and cereals. For the thiamin content of various foods, see Table 1.3.9.7 “Thiamin Content of Various Foods.”
Table 1.3.9.7 Thiamin content of various foods
| Food | Serving | Thiamin (mg) | Percent daily value |
| Breakfast cereals, fortified | 1 serving | 1.5 | 100 |
| White rice, enriched | ½ c. | 1.4 | 73 |
| Pork chop, broiled | 3 oz. | 0.4 | 27 |
| Black beans, boiled | ½ c. | 0.4 | 27 |
| Tuna, cooked | 3 oz. | 0.2 | 13 |
| Brown rice, cooked, not enriched | ½ c. | 0.1 | 7 |
| Whole wheat bread | 1 slice | 0.1 | 7 |
| 2% Milk | 8 oz. | 0.1 | 7 |
| Cheddar cheese | 1 ½ oz | 0 | 0 |
| Apple, sliced | 1 c. | 0 | 0 |
Source: Health Professional Fact Sheet: Thiamin. Office of Dietary Supplements, National Institutes of Health.https://ods.od.nih.gov/factsheets/Thiamin-HealthProfessional/ . Updated February 11, 2016 . Accessed October 5, 2017.
Riboflavin (B2)
Riboflavin is an essential component of flavoproteins, which are coenzymes involved in many metabolic pathways of carbohydrate, lipid, and protein metabolism. Flavoproteins aid in the transfer of electrons in the electron transport chain. Furthermore, the functions of other B-vitamin coenzymes, such as vitamin B6 and folate, are dependent on the actions of flavoproteins. The “flavin” portion of riboflavin gives a bright yellow color to riboflavin, an attribute that helped lead to its discovery as a vitamin. When riboflavin is taken in excess amounts (supplement form) the excess will be excreted through your kidneys and show up in your urine. Although the color may alarm you, it is harmless. There are no adverse effects of high doses of riboflavin from foods or supplements that have been reported.
Riboflavin deficiency, sometimes referred to as ariboflavinosis, is often accompanied by other dietary deficiencies (most notably protein) and can be common in people that suffer from alcoholism. This deficiency will usually also occur in conjunction with deficiencies of other B vitamins because the majority of B vitamins have similar food sources. Its signs and symptoms include dry, scaly skin, cracking of the lips and at the corners of the mouth, sore throat, itchy eyes, and light sensitivity.
Dietary Sources
Riboflavin can be found in a variety of different foods but it is important to remember that it can be destroyed by sunlight. Milk is one of the best sources of riboflavin in the diet and was once delivered and packaged in glass bottles. This packaging has changed to cloudy plastic containers or cardboard to help block the light from destroying the riboflavin in milk. For the riboflavin content of various foods, see Table 1.2.9.8 “Riboflavin Content of Various Foods.”
Table 1.3.9.8 Riboflavin Content of Various Foods
| Food | Serving | Riboflavin (mg) | Percent Daily Value |
| Beef liver | 3 oz. | 2.9 | 171 |
| Breakfast cereals, fortified | 1 serving | 1.7 | 100 |
| Instant oats, fortified | 1 c. | 1.1 | 65 |
| Plain yogurt, fat free | 1 c. | 0.6 | 35 |
| 2% milk | 8 oz. | 0.5 | 29 |
| Beef, tenderloin steak | 3 oz. | 0.4 | 24 |
| Portabella mushrooms, sliced | ½ c. | 0.3 | 18 |
| Almonds, dry roasted | 1 oz. | 0.3 | 18 |
| Egg, scrambled | 1 large | 0.2 | 12 |
| Quinoa | 1 c. | 0.2 | 12 |
| Salmon, canned | 3 oz. | 0.2 | 12 |
| Spinach, raw | 1 c. | 0.1 | 6 |
| Brown rice | ½ c. | 0 | 0 |
Source: Fact Sheet for Health Professionals, Riboflavin. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/Riboflavin-HealthProfessional/. Updated February 11, 2016. Accessed October 22, 2017.
Niacin (B3)
Niacin is a component of the coenzymes NADH and NADPH, which are involved in the catabolism and/or anabolism of carbohydrates, lipids, and proteins. NADH is the predominant electron carrier and transfers electrons to the electron-transport chain to make ATP. NADPH is also required for the anabolic pathways of fatty-acid and cholesterol synthesis. In contrast to other vitamins, niacin can be synthesized by humans from the amino acid tryptophan in an anabolic process requiring enzymes dependent on riboflavin, vitamin B6, and iron. Niacin is made from tryptophan only after tryptophan has met all of its other needs in the body. The contribution of tryptophan-derived niacin to niacin needs in the body varies widely and a few scientific studies have demonstrated that diets high in tryptophan have very little effect on niacin deficiency. Niacin deficiency is commonly known as pellagra and the symptoms include fatigue, decreased appetite, and indigestion. These symptoms are then commonly followed by the four D’s: diarrhea, dermatitis, dementia, and sometimes death.
Figure 1.3.9.10 Conversion of Tryptophan to Niacin
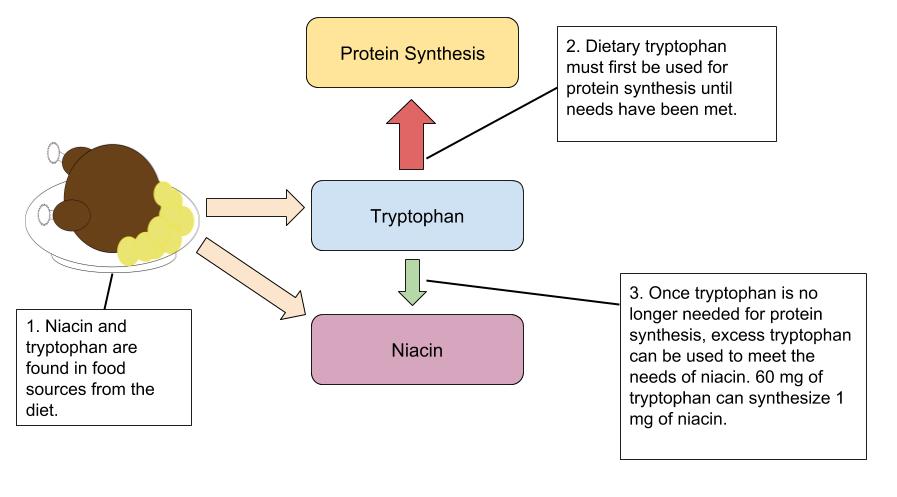
Dietary Sources
Niacin can be found in a variety of different foods such as yeast, meat, poultry, red fish, and cereal. In plants, especially mature grains, niacin can be bound to sugar molecules which can significantly decrease the niacin bioavailability. For the niacin content of various foods, see Table 1.3.9.9 “Niacin Content of Various Foods.”
Table 1.3.9.9 Niacin Content of Various Foods
| Food | Serving | Niacin (mg) | Percent Daily Value |
| Chicken | 3 oz. | 7.3 | 36.5 |
| Tuna | 3 oz. | 8.6 | 43 |
| Turkey | 3 oz. | 10.0 | 50 |
| Salmon | 3 oz. | 8.5 | 42.5 |
| Beef (90% lean) | 3 oz. | 4.4 | 22 |
| Cereal (unfortified) | 1 c. | 5 | 25 |
| Cereal (fortified) | 1 c. | 20 | 100 |
| Peanuts | 1 oz. | 3.8 | 19 |
| Whole wheat bread | 1 slice | 1.3 | 6.5 |
| Coffee | 8 oz. | 0.5 | 2.5 |
Source: Micronutrient Information Center: Niacin. Oregon State University, Linus Pauling Institute. http://lpi.oregonstate.edu/mic/vitamins/niacin. Updated in July 2013. Accessed October 22, 2017.
Pantothenic Acid (B5)
Pantothenic acid forms coenzyme A, which is the main carrier of carbon molecules in a cell.
Coenzyme A is also involved in the synthesis of lipids, cholesterol, and acetylcholine (a neurotransmitter). A Pantothenic Acid deficiency is exceptionally rare. Signs and symptoms include fatigue, irritability, numbness, muscle pain, and cramps. You may have seen pantothenic acid on many ingredients lists for skin and hair care products; however there is no good scientific evidence that pantothenic acid improves human skin or hair.
Dietary Sources
Pantothenic Acid is widely distributed in all types of food, which is why a deficiency in this nutrient is rare. Pantothenic Acid gets its name from the greek word “pantothen” which means “from everywhere.” For the pantothenic acid content of various foods, see Table 1.3.9.10 Pantothenic Acid Content of Various Foods.”
Table 1.3.9.10 Pantothenic Acid Content of Various Foods
| Food | Serving | Pantothenic Acid (mg) | Percent Daily Value |
| Sunflower seeds | 1 oz. | 2 | 20 |
| Fish, trout | 3 oz. | 1.9 | 19 |
| Yogurt, plain nonfat | 8 oz. | 1.6 | 16 |
| Lobster | 3 oz. | 1.4 | 14 |
| Avocado | ½ fruit | 1 | 10 |
| Sweet potato | 1 medium | 1 | 10 |
| Milk | 8 fl oz. | 0.87 | 8.7 |
| Egg | 1 large | 0.7 | 7 |
| Orange | 1 whole | 0.3 | 3 |
| Whole wheat bread | 1 slice | 0. 21 | 2.1 |
Source: Micronutrient Information Center: Pantothenic Acid. Oregon State University, Linus Pauling Institute. http://lpi.oregonstate.edu/mic/vitamins/patothenic-acid . Updated in July 2013. Accessed October 22, 2017.
Biotin
Biotin is required as a coenzyme in the citric acid cycle and in lipid metabolism. It is also required as an enzyme in the synthesis of glucose and some nonessential amino acids. A specific enzyme, biotinidase, is required to release biotin from protein so that it can be absorbed in the gut. There is some bacterial synthesis of biotin that occurs in the colon; however this is not a significant source of biotin. Biotin deficiency is rare, but can be caused by eating large amounts of egg whites over an extended period of time. This is because a protein in egg whites tightly binds to biotin making it unavailable for absorption. A rare genetic disease-causing malfunction of the biotinidase enzyme also results in biotin deficiency. Symptoms of biotin deficiency are similar to those of other B vitamins, but may also include hair loss when severe.
Dietary Sources
Biotin can be found in foods such as eggs, fish, meat, seeds, nuts and certain vegetables. For the pantothenic acid content of various foods, see Table 1.3.9.11 “Biotin Content of Various Foods.”
Table 1.3.9.11 Biotin Content of Various Foods
| Food | Serving | Biotin (mcg) | Percent daily value* |
| Eggs | 1 large | 10 | 33.3 |
| Salmon, canned | 3 oz. | 5 | 16.6 |
| Pork chop | 3 oz. | 3.8 | 12.6 |
| Sunflower seeds | ¼ c. | 2.6 | 8.6 |
| Sweet potato | ½ c. | 2.4 | 8 |
| Almonds | ¼ c. | 1.5 | 5 |
| Tuna, canned | 3 oz. | 0.6 | 2 |
| Broccoli | ½ c. | 0.4 | 1.3 |
| Banana | ½ c. | 0.2 | 0.6 |
| * Current AI used to determine Percent Daily Value |
Source: Fact Sheet for Health Professionals: Biotin. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/Biotin-HealthProfessional/. Updated October 3, 2017. Accessed November 10, 2017.
Vitamin B6 (Pyridoxine)
Vitamin B6 is the coenzyme involved in a wide variety of functions in the body. One major function is the nitrogen transfer between amino acids which plays a role in amino-acid synthesis and catabolism. Also, it functions to release glucose from glycogen in the catabolic pathway of glycogenolysis and is required by enzymes for the synthesis of multiple neurotransmitters and hemoglobin
Vitamin B6 is also a required coenzyme for the synthesis of hemoglobin. A deficiency in vitamin B6 can cause anemia, but it is of a different type than that caused by insufficient folate, cobalamin, or iron; although the symptoms are similar. The size of red blood cells is normal or somewhat smaller but the hemoglobin content is lower. This means each red blood cell has less capacity for carrying oxygen, resulting in muscle weakness, fatigue, and shortness of breath. Other deficiency symptoms of vitamin B6 can cause dermatitis, mouth sores, and confusion.
The vitamin B6 coenzyme is needed for a number of different reactions that are essential for amino acid synthesis, catabolism for energy, and the synthesis of glucose and neurotransmitters.
Vitamin B6 coenzyme is essential for the conversion of amino acid methionine into cysteine. With low levels of Vitamin B6, homocysteine will build up in the blood. High levels of homocysteine increases the risk for heart disease.
Vitamin B6 Toxicity
Currently, there are no adverse effects that have been associated with a high dietary intake of vitamin B6, but large supplemental doses can cause severe nerve impairment. To prevent this from occurring, the UL for adults is set at 100 mg/day.
Dietary Sources
Vitamin B6 can be found in a variety of foods. The richest sources include fish, beef liver and other organ meats, potatoes, and other starchy vegetables and fruits. For the Vitamin B6 content of various foods, see Table 1.3.9.12 “Vitamin B6 Content of Various Foods.”
Table 1.3.9.12 Vitamin B6 Content of Various Foods
| Food | Serving | Vitamin B6 (mg) | Percent Daily Value |
| Chickpeas | 1 c. | 1.1 | 55 |
| Tuna, fresh | 3 oz. | 0.9 | 45 |
| Salmon | 3 oz. | 0.6 | 30 |
| Potatoes | 1 c. | 0.4 | 20 |
| Banana | 1 medium | 0.4 | 20 |
| Ground beef patty | 3 oz. | 0.3 | 10 |
| White rice, enriched | 1 c. | 0.1 | 5 |
| Spinach | ½ c | 0.1 | 5 |
Source: Dietary Supplement Fact Sheet: Vitamin B6. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/VitaminB6-HealthProfessional/. Updates February 11, 2016. Accessed October 22, 2017.
Folate
Folate is a required coenzyme for the synthesis of the amino acid methionine, and for making RNA and DNA. Therefore, rapidly dividing cells are most affected by folate deficiency. Red blood cells, white blood cells, and platelets are continuously being synthesized in the bone marrow from dividing stem cells. When folate is deficient, cells cannot divide normally A consequence of folate deficiency is macrocytic or megaloblastic anemia. Macrocytic and megaloblastic mean “big cell,” and anemia refers to fewer red blood cells or red blood cells containing less hemoglobin. Macrocytic anemia is characterized by larger and fewer red blood cells. It is caused by red blood cells being unable to produce DNA and RNA fast enough—cells grow but do not divide, making them large in size (see Figure 1.3.9.11. “Folate and the Formation of Macrocytic Anemia”).
Figure 1.3.9.11 Folate and the Formation of Macrocytic Anemia
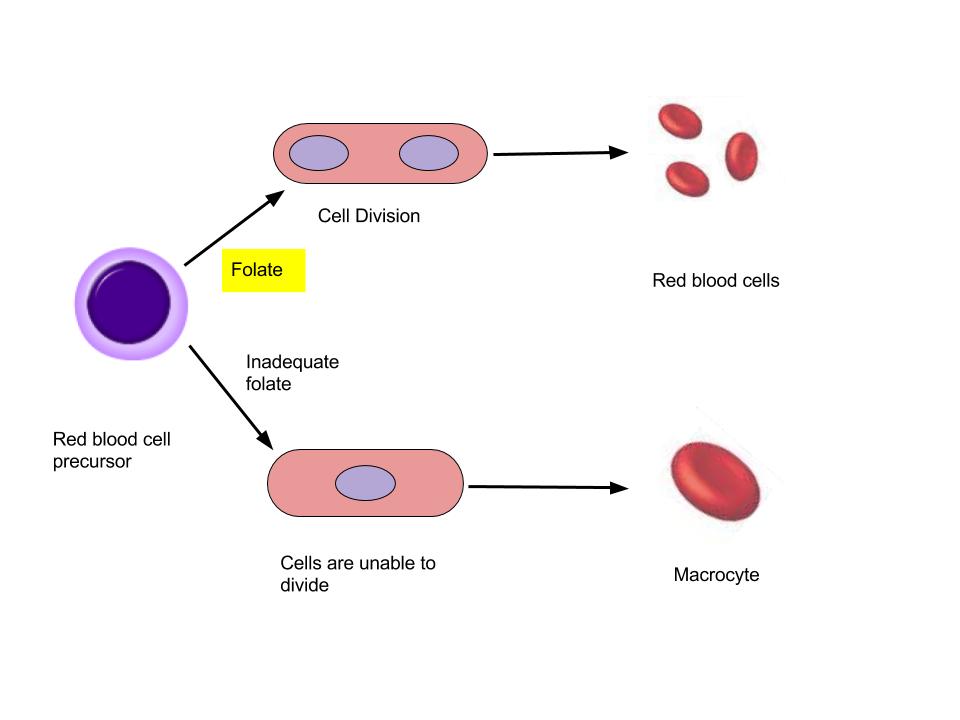
Folate is especially essential for the growth and specialization of cells of the central nervous system. Children whose mothers were folate-deficient during pregnancy have a higher risk of neural-tube birth defects. Folate deficiency is causally linked to the development of spina bifida, a neural-tube defect that occurs when the spine does not completely enclose the spinal cord. Spina bifida can lead to many physical and mental disabilities (Figure 1.3.9.12 “Spina Bifida in Infants”). Observational studies show that the prevalence of neural-tube defects was decreased after the fortification of enriched cereal grain products with folate in 1996 in the United States (and 1998 in Canada) compared to before grain products were fortified with folate.
Additionally, results of clinical trials have demonstrated that neural-tube defects are significantly decreased in the offspring of mothers who began taking folate supplements one month prior to becoming pregnant and throughout the pregnancy. In response to the scientific evidence, the Food and Nutrition Board of the Institute of Medicine (IOM) raised the RDA for folate to 600 micrograms per day for pregnant women. Some were concerned that higher folate intakes may cause colon cancer; however, scientific studies refute this hypothesis.
Figure 1.3.9.12 Spina Bifida in Infants
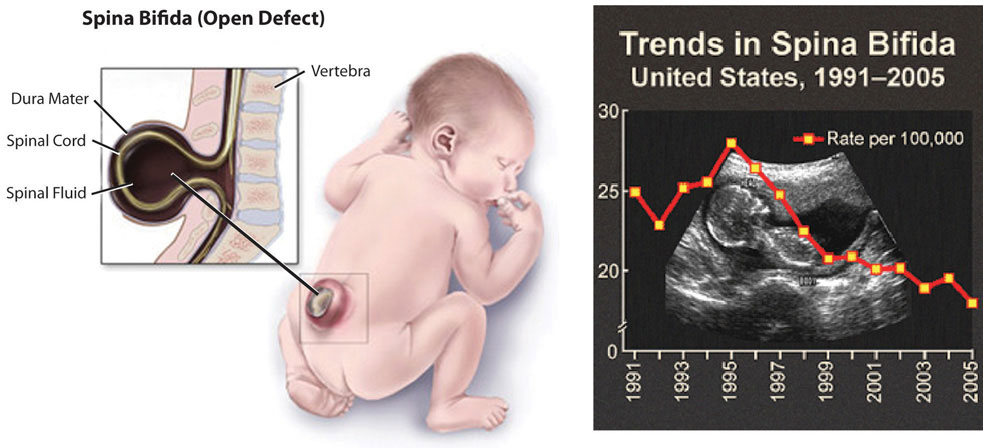
Dietary Reference Intakes
The RDAs and ULs for different age groups for folate are listed in Table 1.3.9.13 “Dietary Reference Intakes for Folate.” Folate is a compound that is found naturally in foods. Folic acid however is the chemical structure form that is used in dietary supplements as well as enriched foods such as grains. The FNB has developed dietary folate equivalents (DFE) to reflect the fact that folic acid is more bioavailable and easily absorbed than folate found in food. The conversions for the different forms are listed below.
1 mcg DFE = 1 mcg food folate
1mcg DFE = 0.6 mcg folic acid from fortified foods or dietary supplements consumed with foods
1 mcg DFE = 0.5 mcg folic acid from dietary supplements taken on an empty stomach
Table 1.3.9.13 Dietary Reference Intakes for Folate
| Age Group | RDA Males and Females mcg DFE/day | UL |
| Infants (0–6 months) | 65* | Not possible to determine |
| Infants (7–12 months) | 80* | Not possible to determine |
| Children (1–3 years) | 150 | 300 |
| Children (4–8 years) | 200 | 400 |
| Children (9–13 years) | 300 | 600 |
| Adolescents (14–18 years) | 400 | 800 |
| Adults (> 19 years) | 400 | 1000 |
| *denotes Adequate Intake |
Source: Dietary Supplement Fact Sheet: Folate. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/. Updated April 20, 2016. Accessed October 22, 2017.
Dietary Sources
Folate is found naturally in a wide variety of food especially in dark leafy vegetables, fruits, and animal products. The U.S. Food and Drug Administration (FDA) began requiring manufacturers to fortify enriched breads, cereals, flours, and cornmeal to increase the consumption of folate in the American diet. For the folate content of various foods, see Table 1.3.9.14 “Folate Content of Various Foods.”
Table 1.3.9.14 Folate Content of Various Foods
| Food | Serving | Folate (mcg DFE) | Percent Daily Value |
| Beef Liver | 3 oz. | 215 | 54 |
| Fortified breakfast cereals | ¾ c. | 400 | 100 |
| Spinach | ½ c. | 131 | 33 |
| White rice, enriched | ½ c. | 90 | 23 |
| Asparagus | 4 spears | 85 | 20 |
| White bread, enriched | 1 slice | 43 | 11 |
| Broccoli | 2 spears | 45 | 10 |
| Avocado | ½ c. | 59 | 15 |
| Orange juice | 6 oz. | 35 | 9 |
| Egg | 1 large | 22 | 6 |
Source: Dietary Supplement Fact Sheet: Folate. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/. Updated April 20, 2016. Accessed October 22, 2017.
Vitamin B12 (Cobalamin)
Vitamin B12 contains cobalt, making it the only vitamin that contains a metal ion. Vitamin B12 is an essential part of coenzymes. It is necessary for fat and protein catabolism, for folate coenzyme function, and for hemoglobin synthesis. An enzyme requiring vitamin B12 is needed by a folate-dependent enzyme to synthesize DNA. Thus, a deficiency in vitamin B12 has similar consequences to health as folate deficiency. In children and adults vitamin B12 deficiency causes macrocytic anemia, and in babies born to cobalamin-deficient mothers there is an increased risk for neural-tube defects. In order for the human body to absorb vitamin B12, the stomach, pancreas, and small intestine must be functioning properly. Cells in the stomach secrete a protein called intrinsic factor that is necessary for vitamin B12 absorption, which occurs in the small intestine. Impairment of secretion of this protein either caused by an autoimmune disease or by chronic inflammation of the stomach (such as that occurring in some people with H.pylori infection), can lead to the disease pernicious anemia, a type of macrocytic anemia. Vitamin B12 malabsorption is most common in the elderly, who may have impaired functioning of digestive organs, a normal consequence of aging. Pernicious anemia is treated by large oral doses of vitamin B12 or by putting the vitamin under the tongue, where it is absorbed into the bloodstream without passing through the intestine. In patients that do not respond to oral or sublingual treatment vitamin B12is given by injection.
Vitamin B12 and folate play key roles in converting homocysteine to amino acid methionine.
High levels of homocysteine in the blood increases the risk for heart disease. Low levels of vitamin B12, folate or vitamin B6 will increase homocysteine levels therefore increasing the risk of heart disease.
When there is a deficiency in vitamin B12 , inactive folate (from food) is unable to be converted to active folate and used in the body for the synthesis of DNA. Folic Acid however (that comes from supplements or fortified foods) is available to be used as active folate in the body without vitamin B12 .Therefore, if there is a deficiency in vitamin B12 macrocytic anemia may occur. With the fortification of foods incorporated into people’s diets, the risk of an individual developing macrocytic anemia is decreased.
Dietary Sources
Vitamin B12 is found naturally in animal products such as fish, meat, poultry, eggs, and milk products. Although vitamin B12 is not generally present in plant foods, fortified breakfast cereals are also a good source of vitamin B12. For the vitamin B12 content of various foods, see Table 1.3.9.15 “Vitamin B12 Content of Various Foods.”
Table 1.3.9.15 Vitamin B12 Content of Various Foods
| Food | Serving | Vitamin B12 (mcg) | Percent Daily Value |
| Clams | 3 oz. | 84.1 | 1,402 |
| Salmon | 3 oz. | 4.8 | 80 |
| Tuna, canned | 3 oz. | 2.5 | 42 |
| Breakfast cereals, fortified | 1 serving | 1.5 | 25 |
| Beef, top sirloin | 3 oz. | 1.4 | 23 |
| Milk, lowfat | 8 fl oz. | 1.2 | 18 |
| Yogurt, lowfat | 8 oz. | 1.1 | 18 |
| Cheese, swiss | 1 oz. | 0.9 | 15 |
| Egg | 1 large | 0.6 | 10 |
Source: Dietary Supplement Fact Sheet: Vitamin B12. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/. Updated February 11, 2016. Accessed October 28, 2017.
Choline
Choline is a water-soluble substance that is not classified as a vitamin because it can be synthesized by the body. However, the synthesis of choline is limited and therefore it is recognized as an essential nutrient. Choline is need to perform functions such as the synthesis of neurotransmitter acetylcholine, the synthesis of phospholipids used to make cell membranes, lipid transport, and also homocysteine metabolism. A deficiency in choline may lead to interfered brain development in the fetus during pregnancy, and in adults cause fatty liver and muscle damage.
Dietary Sources
Choline can be found in a variety of different foods. The main dietary sources of choline in the United States consist of primarily animal based products. For the Choline content of various foods, see Table 1.3.9.16 “Choline Content of Various Foods.”
Table 1.3.9.16 Choline Content of Various Foods
| Food | Serving | Choline (mg) | Percent Daily Value |
| Egg | 1 large | 147 | 27 |
| Soybeans | ½ cup | 107 | 19 |
| Chicken breast | 3 oz. | 72 | 13 |
| Mushrooms, shiitake | ½ c. | 58 | 11 |
| Potatoes | 1 large | 57 | 10 |
| Kidney beans | ½ c. | 45 | 8 |
| Peanuts | ¼ c. | 24 | 4 |
| Brown rice | 1 c. | 19 | 3 |
Source: Fact Sheet for Health Professionals: Choline. Office of Dietary Supplements, National Institutes of Health. https://ods.od.nih.gov/factsheets/Choline-HealthProfessional/. Updated January 25, 2017. Accessed October 28, 2017.
Do B-Vitamin Supplements Provide an Energy Boost?
Although some marketers claim taking a vitamin that contains one-thousand times the daily value of certain B vitamins boosts energy and performance, this is a myth that is not backed by science. The “feeling” of more energy from energy-boosting supplements stems from the high amount of added sugars, caffeine, and other herbal stimulants that accompany the high doses of B vitamins. As discussed, B vitamins are needed to support energy metabolism and growth, but taking in more than required does not supply you with more energy. A great analogy of this phenomenon is the gas in your car. Does it drive faster with a half-tank of gas or a full one? It does not matter; the car drives just as fast as long as it has gas. Similarly, depletion of B vitamins will cause problems in energy metabolism, but having more than is required to run metabolism does not speed it up. Buyers of B-vitamin supplements beware; B vitamins are not stored in the body and all excess will be flushed down the toilet along with the extra money spent.
B vitamins are naturally present in numerous foods, and many other foods are enriched with them. In North America B-vitamin deficiencies are rare; however in the nineteenth century some vitamin-B deficiencies plagued many people in North America. Niacin deficiency, also known as pellagra, was prominent in poorer Americans whose main dietary staple was refined cornmeal. Its symptoms were severe and included diarrhea, dermatitis, dementia, and even death. Some of the health consequences of pellagra are the result of niacin being in insufficient supply to support the body’s metabolic functions.
- Bischoff-Ferrari, HA.,et al. Fracture Prevention with Vitamin D Supplementation: A Meta-Analysis of Randomized Controlled Trials. JAMA. 2005; 293(18), 2257–64. http://jama.ama-assn.org/content/293/18/2257.long. Accessed October 12, 2017. ↵
- Goodman M, Bostlick RM, Kucuk O, Jones DP. Clinical trials of antioxidants as cancer prevention agents: past, present, and future. Free Radic Biol Med. 2011; 51(5), 1068–84. https://www.ncbi.nlm.nih.gov/pubmed/21683786. Accessed October 5, 2017. ↵
- McGinley C, Shafat A. Donnelly AE. Does antioxidant vitamin supplementation protect against muscle damage. Sports Med. 2009; 39(12), 1011–32. https://www.ncbi.nlm.nih.gov/pubmed/19902983. Accessed October 5, 2017. ↵
- Devore EE, et al. Dietary Antioxidants and Long-Term Risk of Dementia. Arch Neurol. 2010; 67(7), 819–25. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2923546/?tool=pubmed. Accessed October 5, 2017. ↵
- Dietary Supplement Fact Sheet: Vitamin E.National Institutes of Health, Office of Dietary Supplements. http://ods.od.nih.gov/factsheets/VitaminE-QuickFacts/. Updated October 11, 2011. Accessed October 5, 2017. ↵
- Mente A, et al. A Systematic Review of the Evidence Supporting a Causal Link between Dietary Factors and Coronary Heart Disease. Arch Intern Med. 2009; 169(7), 659–69. http://archinte.ama-assn.org/cgi/content/full/169/7/659. Accessed October 5, 2017. ↵
- Myint PK, et al. Plasma Vitamin C Concentrations Predict Risk of Incident Stroke Over 10 Years in 20,649 Participants of the European Prospective Investigation into Cancer, Norfolk Prospective Population Study. Am J Clin Nutr. 2008; 87(1), 64–69. http://www.ajcn.org/content/87/1/64.long. Accessed September 22, 2017. ↵
- Douglas RM, et al. Vitamin C for Preventing and Treating the Common Cold. Cochrane Database of Systematic Reviews. 2004; 4. CD000980. http://www.ncbi.nlm.nih.gov/pubmed/15495002?dopt=Abstract. Accessed October 5, 2017. ↵
- Fact Sheets for Health Professionals: Thiamin. National Institute of Health, Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/Thiamin-HealthProfessional/. Updated Feburary 11, 2016. Accessed October 22, 2017. ↵

